BY Erica Rizzo & Eric Beaudoin
The idea of possibly taking a shot to the head is somewhat of an afterthought for 12-year-old hockey defenseman Noah Lastoria. But a shot to the stomach is another story.
Noah’s father, Dominic Lastoria, who just so happens to be the coach of his Pee-Wee hockey team Les Titans de Laval Est, jumps into the conversation to help remind him of the time when he actually sustained a shot to the stomach. It’s a memory Noah would surely like to forget.
“There was also that one time where a guy with a strong slap shot hit me right in the elbow. I felt my joint just…” he says, finishing the anecdote with a poignant “popping” sound.
While the fear of hurting virtually every limb on his body is a concern, the possibility of sustaining a concussion on the ice is not in the realm of fear for Noah: “I would be scared if I got a concussion off ice, but when I’m on the ice I have a helmet, so it protects me.”

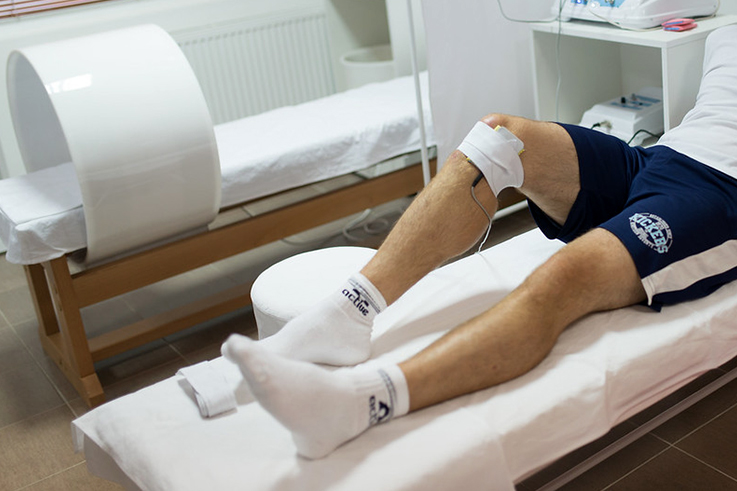
A bad fall on the ice can lead to serious injury, even with protective gear. Photo by RoboMichalec from Pixabay.
Though his helmet does offer a certain amount of superficial protection, the real protection lies in off-ice support personnel.
“At least one of [the coaches and two assistant coaches] had to have the Ambulance Saint-Jean [training],” says Dominic. “So at least one of us is well informed to take care of the situation. But at the arenas there’s always a medical guy—if ever someone gets hurt during a game and it’s serious, they come on the ice and take over.”
This is standard protocol for any level of hockey in Quebec, regardless of the age group.
This protocol is similar to major professional leagues like the NHL, where a team of highly-skilled professionals treat and assess players should they sustain a sport-related concussion (SRC) during a practice or game. It’s just as important for children and teenagers to have access to the same resources, due to the fragility of their still-developing brains.
But this isn’t the reality for all leagues. Jeffrey Caron, an assistant professor at the Université de Montreal and mental performance consultant with the Canadian Sports Psychology Association, highlights that many children’s hockey leagues can’t afford to have medical professionals at games.
“It’s important to note that many youth sports leagues are run by volunteers who do not have medical backgrounds, and many leagues do not have health professionals on-site for each practice and game,” says Caron. “So, some of the problems with concussion diagnosis and management are related to a lack of resources.”
The differences in brains between adults and children can have an effect on the impact of the concussion. Video by Eric Beaudoin.
Children are inherently more vulnerable to brain injury in comparison to adults. A study conducted by Gavin Davis and Laura Purcell, published by the British Journal of Sports Medicine in 2014 revealed that there are significant differences between the brains of adults and children.
This can lead to their susceptibility to establishing “greater injury to the child’s brain, than the adult’s, for the same impact force,” as well as a prolonged recovery period, of which can take longer than 10-14 days in pre-adolescent children.
According to Caron, while the importance of understanding the nuances between a child and an adult brain is important, it is not always paramount for those who are not trained health officials: “It is very problematic if health professionals on the sidelines [such as] athletic therapists, physiotherapists or in the clinic [like] physiotherapists, medical professionals, who are responsible for the care and well-being of athletes with a concussion are not aware of these differences. However, if you are referring to parents […], then I think the messaging becomes a little simpler,” in that their only job is to get them to a hospital where they can be officially assessed.
Another method, and arguably the best protection a hockey player can offer themselves, is to avoid getting body-checked as much as possible. In fact, the main factor preventing Pee-Wee players (age 11-12) from seeing as many concussions in comparison to the (slightly) older Bantam players (age 13-14), is because of the “no body-checking ” rule, implemented in 2013 by Hockey Canada’s Board of Directors.
That rule was recently expanded to include most players under the age of 17.
According to Carolyn Emery, a researcher and co-chair of the Sport Injury Prevention Research Centre in the Faculty of Kinesiology at the University of Calgary, estimated that the eliminating body-checking would prevent over 1,500 concussions, as well as 5,000 other injuries across Canada.
Dominic has noticed that this simple rule change has not only impacted the style of hockey played in Pee-Wee, but has diminished the levels of anxiety in bystanding parents, who would otherwise fear for the health and safety of their child.
Changing the rules around body-checking in hockey can potentially decrease the number of injuries from the sport. Photo by Nenad Stojkovic from Flickr.
“There’s always a risk of concussion, but at their age and their level, there’s less of a danger,” says Dominic. “They’re not going as fast as they are when they’re older—there’s no contact. There’s still danger, but it’s not as bad.”
This does not change the fact that no matter how small a chance a player may have of sustaining a concussion, there’s always still that chance.
Michael Aronis, assistant coach of the Bantam AA Rebelles of the Ligue Intercités Hockey Laurentides Lanaudière Laval, echoes this sentiment.
“The non-contact rule reduces the chances of getting concussions, for sure,” says Aronis. “However, kids will still get them because hockey is an intense sport that is played on ice and so many things are out of everyone’s control.”
In fact, Aronis believes that hockey should be played with contact, at any level. However, he explains that these checks and hits shouldn’t be delivered recklessly.
Instead, there are certain techniques that players are taught in hitting clinics, demonstrative sessions that show “how to hit someone shoulder to shoulder and how to protect yourself,” as well as methods like how to properly roll off a body check, to lessen your “chances of getting hit to the head.”

Some say that parents need to be made more aware of the possible injuries children can have from hockey. Photo by Jill Wellington from Pixabay.
Regardless of how concussions are sustained, or what means are available for initial recognition of a concussion, Caron has two crucial pieces of advice.
The first is stupidly simple: “A concussion is a brain injury. Athletes of any age suspected of brain injury must be assessed by a health professional.”
The second is not directed at players, or their coaches: “It’s very important to make sure that parents are informed about the basics of sport-related concussions,” says Caron.
He adds a reassuring message that “it’s equally important to convey to parents (many of whom are also youth sport coaches) that they do not have to be concussion experts nor do they have to be involved in concussion diagnosis,” with Canadian resources like Parachute offering useful guidelines and instruction for parents.
There may one day be a game where Noah gets lucky and doesn’t take a much-dreaded puck to his stomach or elbow, and instead nails him in the head.
But, his sentiments as to whether or not he would return to hockey, even after the potential trauma and residual fear of a concussion, remain unwavering: “I would still play.”




